May 24, 2021
Diabetes & Gastroparesis | Symptoms, Causes & Treatment
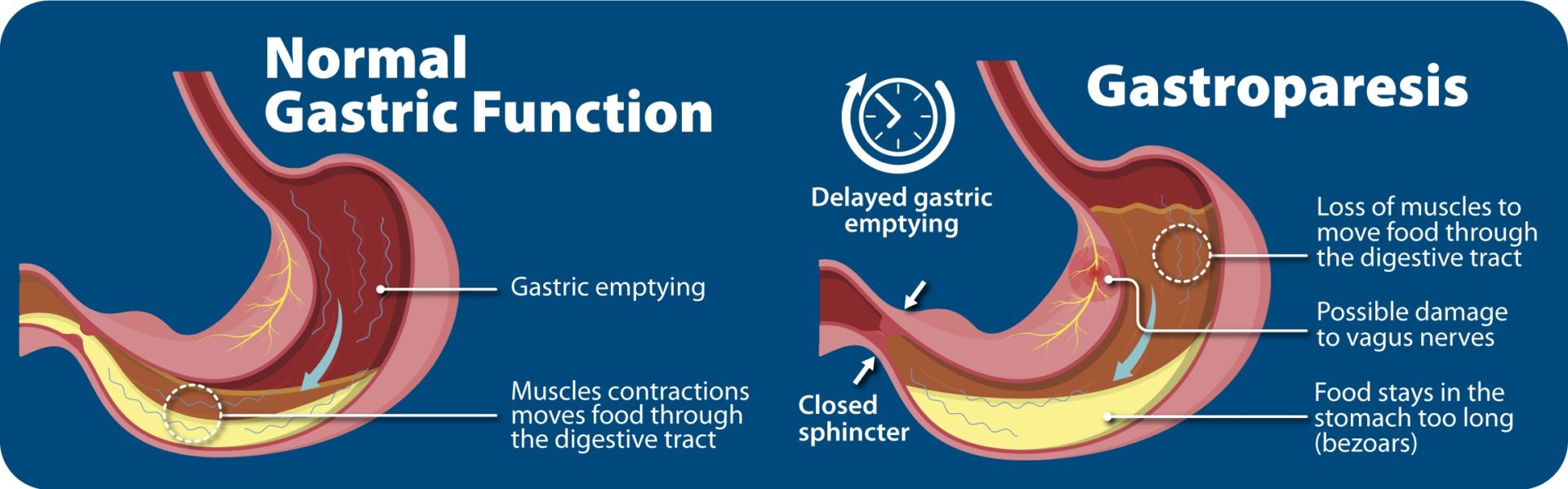
Gastroparesis, also called delayed gastric emptying, occurs when the digestive tract causes food to remain in the stomach for longer than average. Learn more about causes, symptoms and treatments.
Share This Story
Gastroparesis
Worrying about your diabetes diagnosis is enough to make anyone feel queasy – but sometimes, the stress isn’t to blame. If you have a condition called “gastroparesis” (AKA “delayed gastric emptying”), the spontaneous movement of your stomach muscles is slowed or prevented, making it harder for food to move through your digestive tract. Along with its effects on digestion, this condition can result in nausea, abdominal pain, and vomiting.
Gastroparesis isn’t exclusively a complication of diabetes, but people with diabetes can develop delayed gastric emptying as a result of this disease. Read on to learn about risk factors for gastroparesis, symptoms of this complication, and how to treat it if it’s affecting you.
Unsurprisingly enough, most of the symptoms associated with gastroparesis are related to the digestive system. These include:
- Nausea and vomiting
- Feeling full after eating small amounts of food
- Acid reflux
- Abdominal pain/bloating
- Unplanned weight loss
Confusingly enough, gastroparesis may not actually display any observable symptoms. If you do notice any concerning symptoms that could indicate delayed gastric emptying, however, make sure to get in touch with your doctor.
Gastroparesis Risk Factors & Complications
When it’s related to diabetes, gastroparesis is most commonly seen along with type 1 diabetes and in people who have had diabetes for over a decade. That’s not to say it can’t manifest in people with type 2 diabetes or people who have not had diabetes for many years, though. No matter what type of diabetes you have, make sure not to ignore symptoms that could point to this condition.
Other risk factors for gastroparesis include:
- Viral infection
- Surgery on the abdomen or esophagus
- Parkinson’s disease, multiple sclerosis, and other nervous system diseases
- Hypothyroidism
- Sex (women are more likely to experience this condition than men)
Though it often starts as a complication of diabetes, untreated gastroparesis can lead to complications of its own. At best, you could have a lowered quality of life; at worst, you could suffer from malnutrition, dehydration, and unpredictable blood glucose swings. The latter symptom can actively make your diabetes worse – be ready to take steps towards treating gastroparesis as soon as you notice potential symptoms!
What Causes Gastroparesis?
In some cases, it isn’t clear what causes delayed gastric emptying. For the sake of this article, though, we’ll focus on how this condition can arise in relation to diabetes.
Diabetes – especially untreated diabetes – can cause damage to the bodies of people living with this disease. This can appear in the form of neuropathy, kidney damage, damage to extremities, and other symptoms. Along with these forms of damage, diabetes can affect your vagus nerve (the nerve responsible for handling various digestive processes).
When the vagus nerve is damaged, it isn’t able to communicate with a person’s stomach muscles as effectively as it should. Because of this, if a person has gastroparesis, food can stay in their stomach longer than it should.
Gastroparesis Treatment
Before gastroparesis can be treated, your doctor will need to make sure you are actually dealing with this condition. There are a number of methods for diagnosing delayed gastric emptying – these include everything from ultrasound, to gastric emptying tests, to an endoscopy. 
Once you know you’re dealing with gastroparesis, you and your healthcare team will be able to take steps to keep it under control:
Dietary Changes
For a large number of people living with delayed gastric emptying, the most effective form of treatment is making simple dietary changes! If you don’t already work with a dietitian, your doctor might refer you to one to put together a new dietary plan that takes your gastroparesis into account.
Your dietitian could recommend that you make any number of changes to your diet in order to reduce the impact of gastroparesis. These changes could include focusing on low-fat foods, eating cooked fruits and vegetables, eating smaller meals more often, and more. Along with this, your dietitian will be able to recommend specific foods that may be right for you.
Medications
Though making dietary changes can go a long way towards treating gastroparesis, this isn’t enough on its own for everyone. If that’s the case for you, you may need to start taking medications to make it easier for you to deal with this condition.
Some medications used for gastroparesis help stimulate stomach muscles. This category of medications includes erythromycin and metoclopramide. However, both of these medications have risks – metoclopramide is associated with serious side effects, and erythromycin can become less effective over time.
Other medications are used to control the nausea and vomiting associated with gastroparesis. These include the likes of diphenhydramine (Benadryl, etc.), ondansetron (Zofran), and – if these symptoms do not go away – prochlorperazine (Compro).
Surgery
If your gastroparesis has reached the point where you can’t tolerate solid or liquid foods, you may need to have surgery. These procedures can involve the installation of a feeding tube or a gastric venting tube.
Another form of gastroparesis surgery focuses on implanting a device that can electrically stimulate stomach muscles. This is seemingly most helpful for people with diabetic gastroparesis, but scientific findings have been mixed. Currently, the FDA allows these devices to be used by people who can’t control gastroparesis with diet changes or medications.
Is Gastroparesis Prevention Possible?
In cases where the cause of delayed gastric emptying is unknown – that is, idiopathic gastroparesis – there is no way to prevent this condition. On the other hand, if you are concerned about gastroparesis because you have been diagnosed with diabetes, there are some preventative steps you can take against delayed gastric emptying.
Luckily, these steps shouldn’t be too hard to follow – the best way to keep diabetes from damaging your vagus nerve is to keep the disease under control. As always, this involves following a meal plan, getting regular exercise, and taking insulin/other medications as needed.
Summary & Outlook
The consequences of gastroparesis can be severe if you don’t take steps to treat it, but these steps don’t usually need to be all that difficult to follow. By making some smart changes to your diet, you can control gastroparesis instead of letting it control you.
Looking for delicious meals that can make it easier to live with gastroparesis and diabetes? Take a look at our large selection of diabetic-friendly recipes. And don’t forget: US MED can take care of all your diabetes supply needs, so start shopping today!
Disclaimer
This content is for informational purposes only and is not a substitute for medical advice. Check with your healthcare provider before making changes to your health routine.